






 t the end of the 19th century, x-rays represented a major step forward in diagnostic and therapeutic medicine, but then sobered physicians and the public after the hazards of ionizing radiation were detected.
t the end of the 19th century, x-rays represented a major step forward in diagnostic and therapeutic medicine, but then sobered physicians and the public after the hazards of ionizing radiation were detected.
No ionizing radiation is involved in MR imaging. However, because of the recognized problems with x-rays and radioisotope examinations, magnetic resonance imaging and spectroscopy have been intensively examined for possible dangerous side effects.
Any new method in medicine, be it diagnostic or therapeutic, must be thoroughly checked for possible adverse effects — and magnets can have fatal attractions (Figure 18-01).
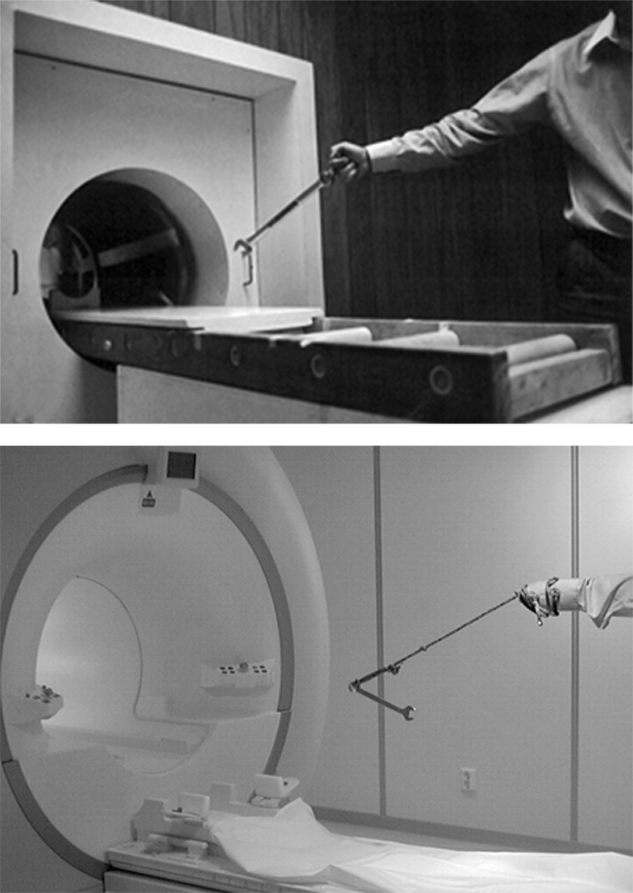
Figure 18-01:
Magnets can have fatal attractions — whether it is low field or high field.
Top: 900 Gauss (0.09 T) at Paul Lauterbur's first whole-body machine, or …
Bottom: … decades later at a clinical 1.5 T machine.
For a long time, only minimal and reversible physiological effects were reported from imaging and spectroscopy equipment operating below 2 Tesla.
Although to date there is no proof of any permanent damages to patients or staff caused by the magnetic or radiofrequency fields of commonly used clinical MR equipment, for some years negative health effects on humans have been increasingly published — mostly concerning ultrahigh machines between 3 T and 7 T and involving both patients and employees.
 During the last 150 years, thousands of papers focusing on the effects or side effects of magnetic or radiofrequency fields have been published. They range from anecdotal reports about therapeutic applications of magnetic fields as published by Zhang et al. [⇒ Zhang 1984], to reports on unwelcome side effects, such as Beischer’s study [⇒ Beischer 1962].
During the last 150 years, thousands of papers focusing on the effects or side effects of magnetic or radiofrequency fields have been published. They range from anecdotal reports about therapeutic applications of magnetic fields as published by Zhang et al. [⇒ Zhang 1984], to reports on unwelcome side effects, such as Beischer’s study [⇒ Beischer 1962].
This overview cannot cover all potential sources of hazards. Numerous reviews of the literature have been put forth immediately after the introduction of MR imaging into clinical routine, e.g., by Budinger as early as 1981 [⇒ Budinger 1981], Rinck [⇒ Rinck 1983], by Persson and Ståhlberg [⇒ Persson 1985]; updates are published every so often, for instance in this textbook or, among others, by Budinger [⇒ Budinger 2016].
Several of the side effects associated with MR are unique to this kind of diagnostic tool; others are similar to hazards of other diagnostic methods. These hazards can affect patients, personnel, and other persons within the field of the magnet.
They can be categorized as incidental and physiological.
 Possible hazards can arise from or be connected to:
Possible hazards can arise from or be connected to:
 static magnetic fields;
static magnetic fields;
 varying magnetic fields (gradient fields);
varying magnetic fields (gradient fields);
 varying magnetic fields (gradient fields);
varying magnetic fields (gradient fields);
and specifically:
 devices necessary to operate the imaging equipment (such as cooling gases) or to ensure the quality of life of the patients (such as intracorporal implants and extracorporal monitors);
devices necessary to operate the imaging equipment (such as cooling gases) or to ensure the quality of life of the patients (such as intracorporal implants and extracorporal monitors);
 conducting loops such as electrical leads or accidental anatomical positions of the patient.
conducting loops such as electrical leads or accidental anatomical positions of the patient.
 There is a wide range of incidental dangers that can lead to accidents (Figures 18-01 and 18-02). Three groups of accidents responsible for more than 90% of all reported injuries to patients and personnel. Nearly all accidents are incidental, caused by negligence — by staff or patient — or the employment of inappropriate or unsuitable equipment or devices. The most common hazards of MR imaging are:
There is a wide range of incidental dangers that can lead to accidents (Figures 18-01 and 18-02). Three groups of accidents responsible for more than 90% of all reported injuries to patients and personnel. Nearly all accidents are incidental, caused by negligence — by staff or patient — or the employment of inappropriate or unsuitable equipment or devices. The most common hazards of MR imaging are:
 Temporary or lasting auditory damage to patients whose ears were not adequately protected (at high or ultrahigh fields);
Temporary or lasting auditory damage to patients whose ears were not adequately protected (at high or ultrahigh fields);
 second or third degree burns or blisters and skin redness caused by different sources;
second or third degree burns or blisters and skin redness caused by different sources;
 injuries caused by ferromagnetic objects ("projectiles") in the magnet room or attached to the patient attracted by the MR equipment.
injuries caused by ferromagnetic objects ("projectiles") in the magnet room or attached to the patient attracted by the MR equipment.
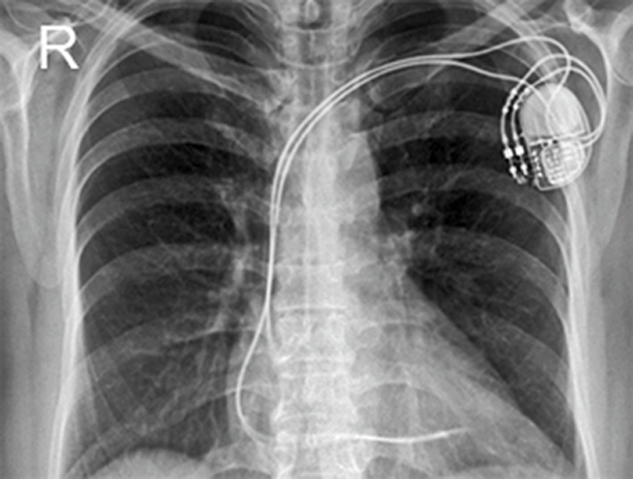
Figure 18-02:
"Are you wearing any metal?"
Repetitive and detailed screening questions prior to an MR imaging examination are the best precaution against harm and injuries.
 The number of contraindications for MR imaging, functional MR, MR spectroscopy, and similar techniques has decreased during the last years. In many instances patient-related devices have been adapted for MR imaging purposes. The contraindications may change from country to country or at different jurisdictions, but adherence to them is strongly recommended. Earlier distinction between absolute and relative contraindications has been replaced by the term "Potential Contraindications". These include:
The number of contraindications for MR imaging, functional MR, MR spectroscopy, and similar techniques has decreased during the last years. In many instances patient-related devices have been adapted for MR imaging purposes. The contraindications may change from country to country or at different jurisdictions, but adherence to them is strongly recommended. Earlier distinction between absolute and relative contraindications has been replaced by the term "Potential Contraindications". These include:
 Electronically, magnetically, and mechanically activated implants: cardiac pacemakers and implantable cardioverter defibrillators;
Electronically, magnetically, and mechanically activated implants: cardiac pacemakers and implantable cardioverter defibrillators;
 lead wires or similar wires;
lead wires or similar wires;
 prosthetic heart valves (in high and ultra-high fields if dehiscence is suspected);
prosthetic heart valves (in high and ultra-high fields if dehiscence is suspected);
 other pacemakers, e.g., for the carotid sinus; entricular-peritoneal shunts, coils and stents, insulin pumps, and nerve stimulators;
other pacemakers, e.g., for the carotid sinus; entricular-peritoneal shunts, coils and stents, insulin pumps, and nerve stimulators;
 stapedial and cochlear implants;
stapedial and cochlear implants;
 hemostatic clips; metallic splinters in the orbit;
hemostatic clips; metallic splinters in the orbit;
 makeup, piercings, and tatoos;
makeup, piercings, and tatoos;
 in certain cases only: pregnancy, congestive heart failure, and claustrophobia.
in certain cases only: pregnancy, congestive heart failure, and claustrophobia.
Details, among them of pregnancy and claustrophobia, are discussed on the following pages.